Las Cruces Comprehensive Rehabilitation and Home Care will soon expand its offering to its patients by adding med spa services, such as facial rejuvenation, Botox fillers and IV hydration and injections. By adding these services, Las Cruces Comprehensive Rehabilitation and Home Care can fulfill the whole body wellness needs of their patients to a greater extent than ever before with continuity of care from the therapy clinic to the med spa. Click to read more!
Continue readingLas Cruces Temporomandibular Joint (TMJ) Therapy
What are TMJ Disorders?
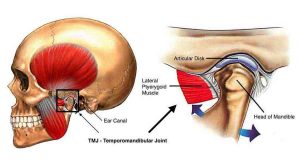 The temporomandibular (tem-puh-roe-man-DIB-u-lur) joint (TMJ) is a joint that connects your jawbone to your skull. TMJ disorders can cause pain in the jaw, neck, ears, head and shoulders. For some people, TMJ disorders can even cause pain or locking of the joint when eating or yawning. According to the Mayo Clinic, “the exact cause of a person’s TMJ disorder is often difficult to determine. Your pain may be due to a combination of factors, such as genetics, arthritis or jaw injury.”
The temporomandibular (tem-puh-roe-man-DIB-u-lur) joint (TMJ) is a joint that connects your jawbone to your skull. TMJ disorders can cause pain in the jaw, neck, ears, head and shoulders. For some people, TMJ disorders can even cause pain or locking of the joint when eating or yawning. According to the Mayo Clinic, “the exact cause of a person’s TMJ disorder is often difficult to determine. Your pain may be due to a combination of factors, such as genetics, arthritis or jaw injury.”
How can physical therapy help with TMJ disorders?
Physical therapy includes a comprehensive evaluation of the patient’s symptoms, medical history and needs. Then the physical therapist will develop and individualized treatment plan to improve and restore normal function of the neck and jaw. Many different types of treatment may be used to help TMJ disorders, including biofeedback, neuromuscular re-education, relaxation techniques, diaphragmatic breathing, exercises to improve range of motion and strength, jaw stabilization and manual therapy. Manual therapy may include Soft Tissue Mobilization or STM, Myofascial Release or MFR, and Trigger Point Release or TP. In addition, posture and ergonomic training and oral habit awareness to reduce clenching and grinding habits can help reduce the stress on the TMJ. Through a combination of joint exercises, massage, breathing exercises, and manual therapy, patients can experience relief from pain and improved quality of life.
Can my dentist help with my TMJ disorder?
Many people may discuss their temporomandibular disorder (TMD) with their dentists; however, many dentists will then refer the patient to do physical therapy to help with the disorder, in addition to encouraging use of a nighttime mouth guard. According to the National Institute of Health, “Although routinely managed by medical and dental practitioners, TMD may be more effectively cared for when physical therapists are involved in the treatment process. Although routinely managed by medical and dental practitioners, TMD may be more effectively cared for when physical therapists are involved in the treatment process.” By discussing your TMJ disorder with your dentist or doctor and seeking physical therapy in addition to that, patients will receive the most effective care for their condition. Physical therapists will work with patients to complete exercises during the session, as well as give patients exercises to work on at home in order to see the most progress in their treatment program. Posture, jaw and neck exercises and stretching are the most common that patients can do at home to further their therapy program.
What should I expect at my fist appointment?
When patients first arrive, they will fill out paperwork about medical history and insurance information. The patient will then undergo an evaluation with a licensed therapist or therapy assistant that will determine the best course of therapy for the individual patient based on their symptoms, medical history and goals for therapy. The patient will then begin exercises that will get them started on their therapy goals. Patients will also be sent with exercises to do at home that will further their progress of their therapy goals.
How long with a course of therapy for TMJ disorders last?
For many people, a course of physical therapy for TMJ disorders may last 6-8 weeks or longer, if needed. Every patient is provided a course of therapy that fits their individual needs and ensures their therapy goals are met and they have relief from their pain.
Find relief today and contact us for TMJ Therapy
Prosthetic Training at Las Cruces Comprehensive Rehabilitation
Las Cruces Comprehensive Rehabilitation offers something that is difficult to find anywhere else in the area: prosthetic training for those requiring a hand and arm prosthesis. Laura Visanko, M.O.T. is an occupational therapist that has been working with hands for 29 years and has received specialized training on working with patients that will be receiving a hand prosthesis. Visanko begins working with patients before they ever receive the prosthesis, helping file insurance paperwork and provide justification for the device, which can be a lengthy and complicated process. Visanko coordinates with the doctor and prosthesis supplier, such as Hanger or PrimeCare. In conjunction with all of this, patients also begin occupational therapy with Visanko that will support their use of the prosthesis once it is received. She works with and supports her patients every step of the way!
 According to the National Center for Biotechnical Information, “majority of all upper-limb amputations are the result of trauma,” but “other common causes of upper-limb loss are vascular/infection, congenital absence, and cancer.” While not using a prosthetic device is an option, patients often find it much easier to rejoin a bi-manual world with the use of some sort of prosthetic device.
According to the National Center for Biotechnical Information, “majority of all upper-limb amputations are the result of trauma,” but “other common causes of upper-limb loss are vascular/infection, congenital absence, and cancer.” While not using a prosthetic device is an option, patients often find it much easier to rejoin a bi-manual world with the use of some sort of prosthetic device.
There are several different types of prosthetic devices that can be used in the case of upper-limb loss. One of these devices is the passive prosthesis. The passive prosthesis is mostly used for the appearance. As passive prosthesis can closely resemble the patient’s sound arm. It does not move on its own, but can be used to restore some balance and for stabilizing and carrying objects. Passive prostheses are often used if the patient does not have significant muscle left in the arm. It is also the lightest option and therefore may be more comfortable. It requires manual repositioning, usually through the use of the sound hand.
Another type of prosthesis is the myoelectric prosthesis, such as the iLimb. Myoelectric prostheses are body-powered, meaning that the movement of the device is connected to a body part. Electrodes are used from the bicep or tricep to activate the myoelectric hand. A myoelectric hand is multi-articulating and each digit is individually powered. In order to use a myoelectric prosthesis, patients must have some muscle tissue left in their remaining arm in order to activate the myoelectric hand. Some of the benefits of the myoelectric prosthesis are that it has multiple grip patterns and effortless strength. It can also be the most intuitive and physiologically natural option. In addition, it can be covered with silicone that can closely resemble a patient’s natural skin.
Patients are first assessed to determine what kind of prosthetic device would be best for their particular situation. At this initial evaluation, their strength of remaining muscles is assessed, as well as their range of motion. Patients with a strength grade of at least 3-4 may qualify for a myoelectric prosthesis. Those with little to no muscle left in their arm will likely be fitted with a passive prosthesis.
Before the patient even receives their prosthesis, Visanko works with them both physically and mentally preparing them for it. She says it’s important for the patient to work on the mindset of returning to a bi-manual world. She talks to them about their activities of daily living (ADL) and any adaptive equipment they may need in order to perform these daily tasks, such as dressing, cooking, chores, driving and even creative activities they enjoy, such as painting or drawing. In addition, the exercises they do creates endorphins, which can help relieve pain, reduce stress and help the patient’s overall wellness.
The patient must also be prepared physically. They work on core strength and posture, as well as scapular stabilization. Visanko works with patients on restoring range of motion and neuromuscular strength using light resistance. Patients must also be prepared to strengthen the distal site, in order to carry the weight of the prosthesis. Weights are used on the distal site in order to prepare the patient for this. In addition, Visanko addresses issues such as scar tissue, hypersensitivity, swelling and phantom pain, where the patient still feels the pain of the lost extremity. One of the therapies she uses to address this is mirror visual feedback.
When the patient finally gets their prosthesis, Visanko helps them get comfortable with it, learn to don it themselves and of course, learn how to use it in everyday life. In the case of a myoelectric prosthesis, the patient first learns to open and close it. Then they learn prehension patterns, such as lateral pinch and tripod pinch, which is used for picking things up. Finally they learn to program certain positions that they know they will use often. Lastly, the patient transitions from programming into function, by using the prosthesis for everyday tasks, such as pulling up their pants, holding jars, cutting vegetables, etc…as well as creative activities or work they once engaged in. It is in this final transition that patients are able to find freedom in returning to the bi-manual world and the activities and work they once enjoyed.
Patients with limb loss can find additional support from organizations such as the Amputee Coalition and the Amputation Foundation. They can also find additional resources at the National Limb Loss Information Center. For more information about prosthetic training or working with Laura Visanko, contact Las Cruces Comprehensive Rehabilitation at (575) 522-0484.
Aquatic Therapy in Las Cruces
What is aquatic therapy?
Aquatic therapy is a physical therapy that is administered in a pool of water for the purpose of relieving pain and pressure on various joints, organs and other body parts. The aquatic therapy pool at Las Cruces Comprehensive Rehabilitation is a therapeutic 92 degree salt water pool that can be used for all types of physical therapy for people with many different conditions and injuries
Cardiopulmonary Rehabilitation Therapy in Las Cruces
What is cardiopulmonary therapy?
Las Cruces Comprehensive Rehabilitation offers licensed pulmonary rehabilitation for patients who have chronic lung disease, such as Chronic Obstructive Pulmonary Disease (COPD) or Pulmonary Fibrosis. Pulmonary rehabilitation can also be beneficial for patients with bronchitis, emphysema, asthma, cystic fibrosis, and other diseases and conditions that affect the lungs. It can even be beneficial for patients that go through surgery due to lung cancer or a lung transplant. Through pulmonary rehabilitation, patients can have hope for regaining lung function, building strength and improving quality of life. Many patients with chronic lung disease do not know about pulmonary rehabilitation, but Las Cruces Comprehensive Rehabilitation wants to change that, so that they can help more people with chronic lung disease can improve their quality of life and overall health. In addition, Las Cruces Comprehensive Rehabilitation can also see heart patients whose doctors recommend cardiopulmonary therapy. Las Cruces Comprehensive Rehabilitation offers the best quality of service with experienced, licensed therapists to provide each patient with a quality of care they may not receive elsewhere.
Continue readingLas Cruces Physical Therapy offered by Las Cruces Comprehensive Rehabilitation
Las Cruces Comprehensive Rehabilitation offers all types of physical therapy, including orthopedic, aquatic, TMJ, hand and physical therapy to support just about any body part that has limited range of motion due to surgery or injury. Every patient that begins a course of therapy at Las Cruces Comprehensive Rehabilitation will be seen by a physical therapist and a physical therapy assistant. Each of their physical therapists have more than 15 years of experience. By working with a highly experienced physical therapist, each patient is receiving the highest level of care, with customized therapy to address each individual’s needs. This high level of experience is what sets Las Cruces Comprehensive Rehabilitation apart from the rest.
Continue reading